We’ve all seen how difficult it can be to be on the organ transplant list. Most of those on the list need a kidney, roughly 90% in fact. However, several others need hearts. A new study has now found a way to hopefully expand the donor pool for hearts. How? Well, through reanimated hearts.
The study/medical trial found that the idea of “reanimating” the heart of an organ donor can work just as efficiently as the standard approach to collecting hearts for transplantation. The researchers found that if this method is widely applied, it would increase the heart donor pool by roughly 30%.
While 30% may not seem like a big number, in terms of organ donation, it’s truly massive.
Dr. Jacob Schroder, a Transplant Surgeon at the Duke University School of Medicine, was who led the study. He told the Associated Press about the findings of their study:
“Honestly if we could snap our fingers and just get people to use this, I think it probably would go up even more than that. This really should be standard of care.”
Some might question why this is important. Moreover, they question what the big deal is behind the “standard approach” as well as the idea of reanimating something at all. Let’s examine that.
How Heart Donation Normally Works
It is important to understand how heart donation works in the normal sense. Because it’ll make the new method easier to understand. You’ll also see why the Duke University study is so critical.
Most transplanted hearts actually come from brain-dead donors who have died due to a complete loss of brain activity. That is otherwise known as “donation after brain death” or DBD. This is important because it means from a circulatory standpoint, they are relatively fine.
This means their heart never stopped, but the person is still effectively dead. That is when families have to decide to allow the person’s life to end, which is often inside the hospital itself. If the person dies and happens to be an organ donor, their organs can be used to help others.
If the person is declared dead before their heart stops beating, then that heart can be used for transplantation purposes. That is because the heart is still perfused with oxygen-rich blood. Therefore, not yet damaged due to any lack of oxygen. Which is pretty critical here.
The heart will then be flushed with preservation solution and placed in an ice-filled cooler. Then it’ll be rushed to the person who needs it.
The Study’s Findings
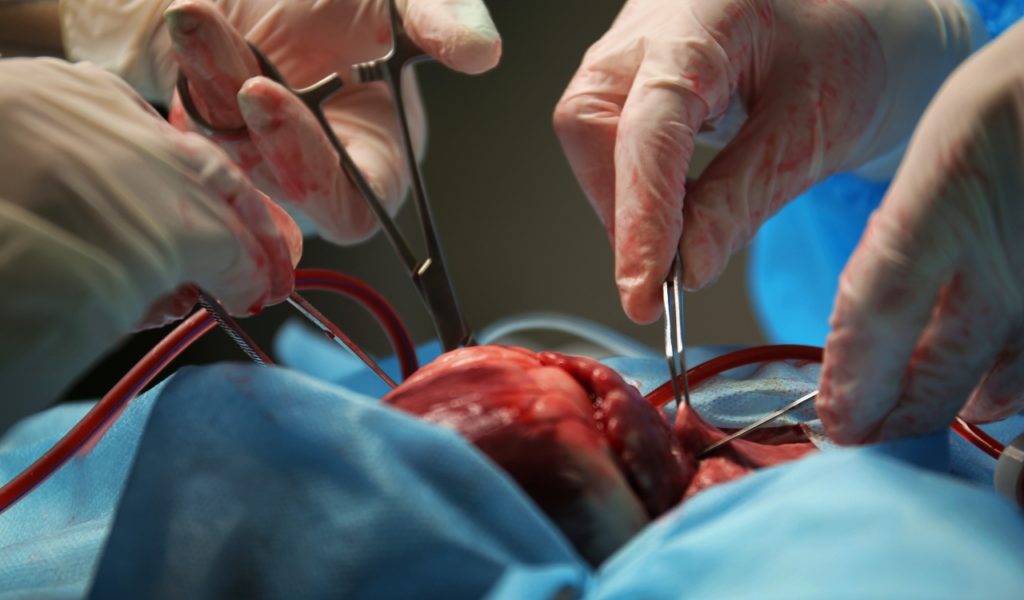
The team published their results in The New England Journal of Medicine back on June 8th. This is one of the most reputable medical journals in the world today.
In their discussion about their findings, they mentioned how doctors referenced the survival rates of transplant recipients who got hearts from donors that were brain-dead. Then they compared them with those who received a heart from those who died from a circulatory death.
A total of 166 United States-based heart transplant patients were included in the university’s primary analysis. 86 were in the brain-dead group & 80 were in the circulatory-death group.
Six months post-surgery, the brain-dead group had a 90% survival rate while the circulatory group actually had a 94% survival rate. That suggested that donation after circulatory dead or DCD is equally viable when it comes to heart transplants.
Plus, let’s not overlook how the reanimated heart concept in reference to using circulatory-dead hearts showed a slightly better survival rate too. This should prove how important a heart can be even when we used to think it was no longer useful.
A reanimated heart is, quite literally, a lifesaver. How can this be done though?
The Reanimated Hearts Difference
Reanimated hearts or the process of DCD is made possible by “extracorporeal machine perfusion.” This involves hooking up the donor organ to a machine that pumps blood and nutrients through its tissues.
The new trial tested a perfusion system called the Organ Care System Heart, which is made by TransMedics. For transparency purposes, you should know that this trial was funded by TransMedics too.
Their system warms the blood that it can pump through the donor heart, as compared with other perfusion systems. Those still require the organ to remain cooled as part of the preservation process.
While the two groups did have a similar survival rate at six months, the DCD group actually had higher rates of moderate to severe primary graft dysfunction. This is when one or both of the heart’s ventricles show dangerous dysfunction within 24 hours of the transplantation surgery.
However, none of the DCD crew had primary graft failure that resulted in transplantation. Meanwhile, two people in the traditional transplant group did. Overall, the rate of serious adverse events was very low and similar in both groups. At least when assessing them at the 30-day post-surgery mark.
The Importance Of This Study/Trial
This new medical trial/study involved several medical centers. The information found here only helped to build upon evidence in favor of DCD. Initially, this was drawn from isolated cases and small trials performed at single centers in places like Australia & the United Kingdom.
Historically, one of the biggest issues involved in all of this was the cost. Back in 2019, the Director of Cardiac Transplantation at the Sandra Atlas Bass Heart Hospital, Dr. Brian Lima, told Live Science that very few studies had compared perfusion with standard cold storage.
This meant that there wasn’t any type of major data that existed which could convince hospitals to make the expensive switch nationwide.
At one point, doctors at the Duke University Medical Center had just performed the nation’s first adult heart transplant, with a “reanimated” organ. Following this major procedure, Lima suggested that perfusion could soon become the standard of care. This all came full circle here.
Reanimated hearts could become normalized very soon. However, reanimated organs overall could be too. Likely lowering the transplant list total from over 100,000 to less than 70,000. Again, 30% might not seem like a huge number but when you think of it in terms of 30,000 lives….that number is massive.
References:
https://edition.cnn.com/2019/12/03/health/dcd-heart-transplant-trnd/index.html
https://www.livescience.com/how-long-can-donated-organs-last-before-transplant.html